Medicare Beneficiary Identifier (MBI)
These frequently asked questions (FAQ) provide information regarding Medicare Beneficiary Identifiers (MBIs).
Requests to change a Medicare Beneficiary Identifier (MBI) can occur if a Medicare beneficiary, their authorized representative, or CMS suspects a number is compromised. If CMS reissues MBIs, it is possible your patients will seek care before receiving a new card with their new MBI.
Your patient’s MBI may have changed if you receive an eligibility transaction error code (AAA 72) of “invalid member ID,” or the eServices Eligibility Inquiry message, “The beneficiary you requested cannot be found. Please verify your information.”
When an MBI changes, the beneficiary is advised to share the new MBI with their providers. If you cannot obtain the new MBI from the patient, you can get it from the eServices MBI Lookup Tool. Sign up for eServices now to use the tool. Instructions for using the MBI Lookup Tool can be found in the eServices User Manual (PDF, 8.59 MB). The Provider Contact Center cannot disclose the new MBI.
The following scenarios can help you determine when to use the old or new MBIs:
Fee-For-Service (FFS) claims submissions with:
- Dates of service before the MBI change date — use old or new MBIs
- Span-date claims with a “From Date” before the MBI change date — use old or new MBIs
- Dates of service that are entirely on or after the effective date of the MBI change – use new MBIs
FFS eligibility transactions when the:
- Inquiry uses new MBI — we will return all eligibility data
- Inquiry uses the old MBI and request date or date range overlap the active period for the old MBI — we will return all eligibility data. We will also return the old MBI termination date.
- Inquiry uses the old MBI and request date or date range are entirely on or after the effective date of the new MBI — we will return an error code (AAA 72) of “invalid member ID”
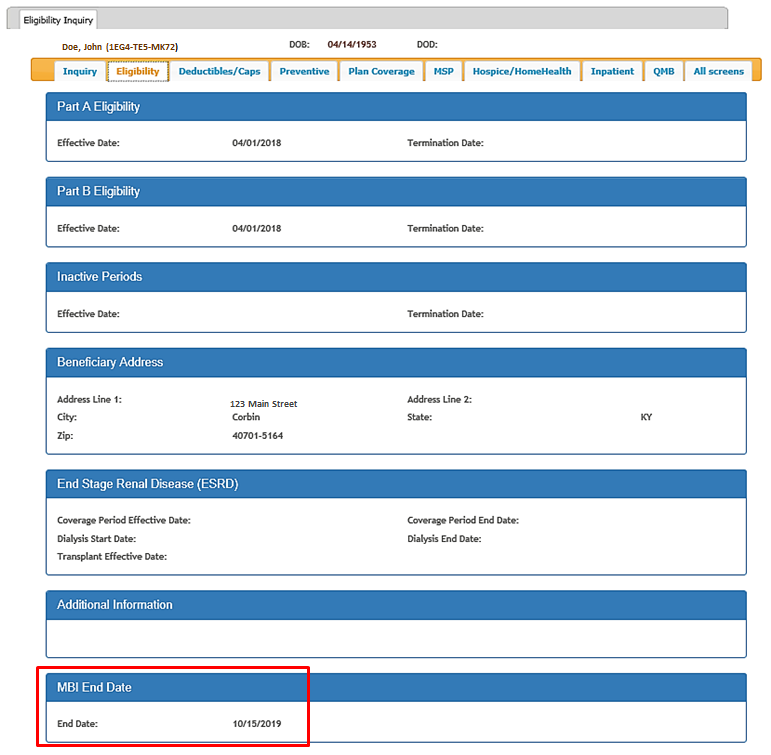
You can find the termination date of the old MBI by doing a historic eligibility search in eServices. The termination date will be returned in the MBI End Date field of the Eligibility tab.
Last Reviewed: 03/07/2025